Hot flashes are one of the most common symptoms experienced by women around the time of menopause. In fact, approximately half of all perimenopausal women and 75 - 85% of all postmenopausal women experience hot flashes.
While the onset, duration, frequency, and severity of hot flashes varies greatly between women, hot flashes often begin in the years before a woman's last period and can last anywhere from six months to fifteen years.
Hot flashes are caused by hormonal fluctuations that occur during the menopausal transition. Fortunately, treating this underlying hormonal imbalance naturally and making simple lifestyle changes is all that most women need to manage this symptom. Continue reading to learn more about hot flashes, their symptoms, causes, management, and treatments.

About Hot Flashes
What Are Hot Flashes?
Hot flashes, also called "hot flushes", are a vasomotor symptom of menopause. This means that hot flashes can disrupt the normal regulation of blood vessels, resulting in intense heat, perspiration, and other symptoms that can range from mild to severe.
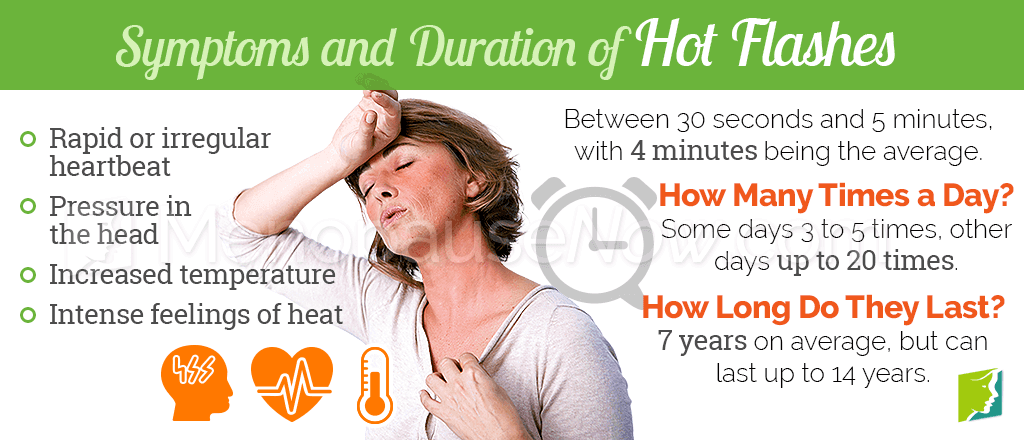
The duration and frequency of hot flashes varies from woman to woman. Hot flashes can occur at any time of the day or night, though they are often called night sweats when they happen during sleeping hours.
Women with menopause-related hot flashes will usually experience a consistent and unique pattern of symptoms. Some women experience mild symptoms of hot flashes infrequently, while others experience more severe symptoms multiple times each day.
Signs and Symptoms of Hot Flashes
The following are the most common signs and symptoms of hot flashes:
- Sudden, intense feelings of heat. This can appear in the face, neck, arms, torso, and sometimes the whole body.
- Rapid or irregular heartbeat and pulse. Heart palpitations may occur.
- Flushing. This symptom is particularly prevalent in lighter-skinned women.
- Perspiration. Sweating can range from mild to profuse.
- Cold chills. This often follow hot flashes, though sometimes women experience only the chill.
- Sleep disturbances. Night sweats can disrupt sleep and lead to fatigue or insomnia.
- Other symptoms. Nausea, dizziness, anxiety, and headaches are other possible symptoms associated with hot flashes.
While each woman will experience the symptoms of hot flashes in a pattern that is unique to her, some women are at a greater risk for more severe and prolonged hot flashes. Women taking the breast cancer treatment drug tamoxifen may experience more severe and prolonged hot flashes. Additionally, women who have total hysterectomies will often experience hot flashes more severely and for a longer duration.
Click on the following link to read more information about hot flashes, or continue reading below to learn more about the causes of hot flashes.
Causes of Hot Flashes
Hormonal Causes
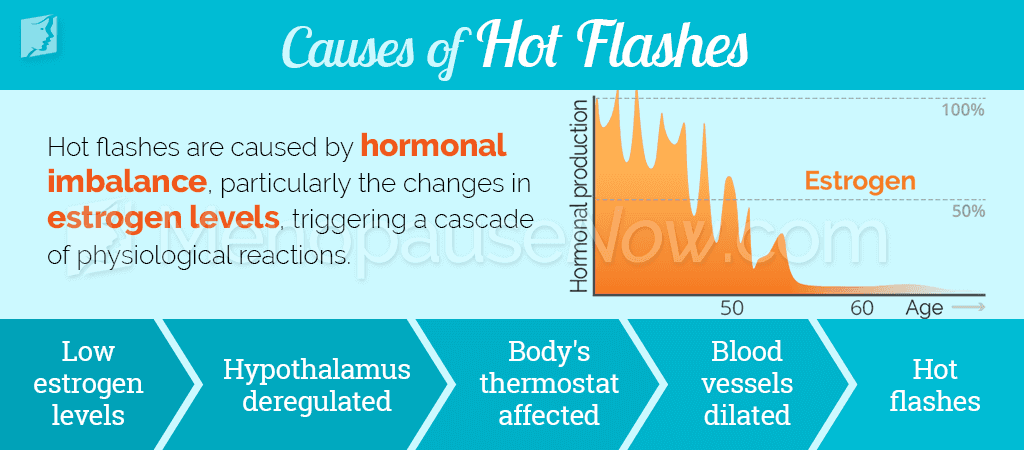
The most common cause of hot flashes in menopausal women is changing levels of estrogen in the body. Estrogen has a direct effect on the hypothalamus, the part of the brain responsible for controlling appetite, sleep, and body temperature.
Lowered levels of estrogen confuse the hypothalamus, causing it to inaccurately sense that the body is overheating. This provokes an internal chain of reactions that women experience as "hot flashes".
In addition to these completely normal hormonal causes of hot flashes, other medical conditions can also cause hot flashes.
Other Causes of Hot Flashes
Certain medical conditions and medications can sometimes cause a person to experience hot flashes. For this reason, women for whom menopause is unlikely or women with other unexplained symptoms should consult a doctor to rule out these other potential causes of hot flashes.
Diseases That Can Cause Hot Flashes
- Panic disorder
- Infection
- Obesity
- Diabetes
- Hyperhidrosis
- Thyroid disease
- Cancer
Medications That Can Cause Hot Flashes
- Raloxifene (osteoporosis drug)
- Tamoxifen (breast cancer drug)
- Gonadotropin analogues (e.g., nafarelin)
Click on the following link to read more information about the causes of hot flashes, or keep reading to learn about managing hot flashes through simple measures, including the avoidance of common hot flash triggers.
Managing Hot Flashes
Thankfully, women who experience hot flashes during menopause have several ways to manage them in order to reduce their frequency and severity. In many cases, simple steps can be taken throughout the day to reduce hot flashes or prevent them altogether. Also, avoiding the common triggers of hot flashes is another important way to combat them.
Simple daily changes that can greatly help a menopausal woman manage hot flashes include:
- Considering air conditioning, ceiling and floor fans, and even small personal handheld fans
- Avoiding being rushed, since it can quickly raise the body's temperature and trigger a hot flash
- Keeping ice water or another cold beverage on hand during the day and night
- Taking a cool shower before bed
- Using cotton sheets and avoiding silk or synthetics
- Keeping a cold pack under or near the pillow and turning the pillow often to keep cool

In addition to making these simple changes, avoiding hot flash triggers can significantly help a woman manage hot flashes.
Common Triggers:
- Warm environments (i.e., hot weather, saunas)
- Devices that give off heat (e.g., fireplaces, hair dryers, heaters)
- Stress
- Anxiety
- Hot and spicy foods and drinks
- Smoking cigarettes
- Overconsumption of caffeine, alcohol, and sugar
- Diet pills
Making minor daily changes and avoiding triggers can make a huge difference for many menopausal women who are trying to manage hot flashes. While these measures often help to reduce the frequency and intensity of hot flashes, they are unable to treat the root of the problem, which is a hormonal imbalance.
Click on the following link to read more information on managing hot flashes, or continue reading below to learn more about the treatments for hot flashes.
Hot Flashes Treatments
If the simple management techniques outlined above are not bringing about relief, there are other treatment measures that can be followed.
Health Tips for Fighting Hot Flashes:
- Practice slow, diaphragmatic breathing
- Eat a balanced diet
- Aim for a vitamin E intake of 800mg/day
- Consider B vitamin levels
- Increase soy protein intake
- Exercise regularly
- Consider meditation or yoga
Daily behaviors can have a significant impact on a woman's experience of hot flashes. For example, eating a spicy dinner or having too many glasses of wine can trigger hot flashes. Increased stress due to work pressure or family obligations can also set a hot flash into motion. Lifestyle adjustments are two-pronged: some strategies focus on avoiding triggers, while others concentrate on increasing overall health - some overlap exists between these two.

It is most logical, as well as safest, to begin with the least invasive lifestyle changes first, and then progress on to other measures if these are not working. Given the fact that at heart, hot flashes are a hormonal issue, it is most effective to address the problem at the source. Natural and alternative remedies are a safe and easy way to balance hormone levels, particularly in conjunction with lifestyle changes to promote overall health.
In more drastic cases, it may be advisable to seek surgical or pharmaceutical treatments, though these are more risky in terms of side effects and should be approached with caution. In addition to hormone replacement therapy (HRT), several other pharmaceutical drugs may be effective hot flash treatment options. These drugs include:
- Selective serotonin reuptake inhibitors (SSRIs)
- Blood pressure medications
- Mild sedatives
- Seizure medications
It is important to keep in mind that while all of these drugs have the potential to assist in hot flash relief, they all carry a risk of side effects, some of which may outweigh any potential benefits. Click on the following link to read and learn more specifics about the different options for the treatment of hot flashes.
Sources
- "Hot flashes ... in January". Canadian Medical Association Journal. 2004: 170 (1).
- National Health Service UK. (2015). Hot flushes: how to cope. Retrieved March 15, 2016, from http://www.nhs.uk/Livewell/menopause/Pages/hot-flushes.aspx
- National Institute on Aging. (2015). What Can You Do for Hot Flashes and Other Menopausal Symptoms. Retrieved March 15, 2016, from https://www.nia.nih.gov/health/publication/menopause-time-change/what-can-you-do-hot-flashes-and-other-menopausal-symptoms
- Sikon, Andrea and Holly Thacker M.D. "Treatment for Menopausal Hot Flashes". Cleveland Clinic Journal of Medicine. July 2004: 71 (7).
- Thurston, R.C. & Joffe, H. (2011). Vasomotor Symptoms and Menopause: Findings from the Study of Women's Health Across the Nation. Obstetrics and Gynecology Clinics of North America, 38(3), 489-501. doi: 10.1016/j.ogc.2011.05.006